Regulatory affairs has never been a static field, but the pace of change heading into 2026 is something else entirely. From AI-driven submission processes to evolving global harmonisation efforts, the future of regulatory affairs is being reshaped by technology, policy reform, and rising expectations around data transparency. For professionals working in regulated industries, accounting, financial services, legal, healthcare, these shifts aren’t abstract. They directly affect how you manage compliance, onboard clients, and report to governing bodies.
What’s driving this? A combination of factors. Regulators worldwide are modernising their own systems, expecting faster digital submissions and more granular data. At the same time, businesses are under pressure to do more with less, automating manual compliance workflows that used to eat up hours every week. In Australia specifically, upcoming AUSTRAC AML/CTF obligations for accountants and other professional services are accelerating the need to rethink how regulatory processes fit into day-to-day operations.
At StackGo, we build integration tools, like IdentityCheck, that let regulated businesses run identity verification and KYC/AML checks directly from their existing software, without switching platforms or stitching together unreliable workarounds. It’s why we pay close attention to where regulatory affairs is heading: the trends below shape what our customers need from their compliance stack tomorrow.
Here are 12 trends worth watching this year.
1. Embed KYC and AML checks inside core systems
The compliance landscape is shifting fast, and manual identity verification workflows are becoming a liability rather than a safeguard. Businesses that still run KYC and AML checks through separate portals, spreadsheets, or disconnected tools are carrying real risk: missed steps, inconsistent records, and audit gaps that regulators notice. Embedding these checks directly into the systems your team already works in is no longer a nice-to-have upgrade.
Why integrated compliance now wins over stand-alone tools
Running KYC and AML verification through a stand-alone tool means your team switches contexts, copy-pastes data, and manually updates records. That creates version control issues and opens the door to human error at every handover point. Integrated compliance tools, by contrast, pull contact data from your CRM, run the check, and write the verified outcome back automatically. Your team stays in one place, and the compliance record is built into the workflow rather than bolted on afterward.
What regulators and auditors expect to see in 2026
Regulators are no longer satisfied with a folder of PDFs as evidence of compliance. In 2026, AUSTRAC and the Tax Practitioners Board (TPB) expect businesses to demonstrate that their verification processes are systematic, consistent, and tied directly to client records. That means showing a clear audit trail: who was verified, when, by what method, and what the outcome was. Spotty or manual record-keeping raises flags during reviews, and Australian accounting firms in particular face growing scrutiny as the new AML/CTF obligations for professional services take hold.
If your compliance records live in a separate system from your client data, you are creating a reconciliation problem that auditors will find before you do.
How integrated identity checks reduce risk and rework
When verification runs inside your core system, duplicate data entry disappears. Your team is not re-keying names, addresses, or document numbers into a separate portal. You also reduce the risk of checking the wrong version of a record, a common problem when client data is spread across multiple platforms. Integrated checks also make remediation faster: if a check fails or flags, the outcome is already attached to the right contact, and your team can act without hunting through separate systems.
Where StackGo fits for identity verification in Australia
StackGo’s IdentityCheck product is built around this exact problem. It connects directly to your CRM, reads the contact information already stored there, runs an identity and AML check across more than 200 countries and 10,000 document types, and writes the verified result back to the contact record. No new software to learn, no manual data transfer, and no PII stored in your CRM. For Australian accounting firms preparing for AUSTRAC obligations, that kind of embedded, auditable workflow is what the future of regulatory affairs looks like in practice.
2. Use AI in regulatory work with proof and controls
AI is moving from experimental to operational inside regulatory teams, but adoption without governance is creating new compliance exposure. The future of regulatory affairs depends on teams using AI in ways they can explain, document, and defend to health authorities.
Where AI adds value across submissions, labelling, and intelligence
Teams are already using AI to cut the time spent on literature screening, gap analysis, and label consistency checks. Submission writing, signal detection, and competitive intelligence work are also seeing real efficiency gains where AI handles volume tasks so your team can focus on judgment calls.
What health authorities expect for AI credibility and traceability
Regulators want to know what AI tool was used, what data it processed, and how a human reviewed the output before it entered a submission. Authorities including the FDA and EMA have both published guidance signalling that AI-assisted content needs clear traceability. If you cannot show the review chain, your submission credibility suffers.
Document every AI-assisted step the same way you would document any other critical review in your quality system.
How teams set governance, human oversight, and audit trails
Your AI governance framework needs to sit inside your existing quality management system, not alongside it. Define which tasks AI can support, who signs off on AI outputs, and how those reviews get recorded. Version-controlled logs of AI tool use protect you during inspections.
How to handle model change over the product lifecycle
Models update frequently, and that creates a change control problem your regulatory team needs to own. When a vendor updates their model, you need to assess whether outputs remain consistent with previously accepted submissions, and document that assessment clearly in your change records.
3. Shift from documents to structured data and APIs
Regulatory submissions built on static PDFs are losing ground fast. The future of regulatory affairs depends on structured data that systems can read, query, and reuse, not documents that require manual review every time a question arises.
Why structured content replaces static PDFs
PDFs lock information inside a fixed format. Regulators and agencies increasingly need to extract, compare, and analyse data across submissions without pulling them apart manually. Structured content standards let you build submissions that health authorities can process programmatically, reducing back-and-forth and speeding up review timelines.
What changes with eCTD evolution and data standards
The eCTD standard is evolving toward richer metadata and machine-readable data packages. Agencies including the FDA and EMA are pushing for submissions that carry structured clinical and non-clinical data alongside documents. Your submission architecture needs to account for IDMP, SPL, and linked data standards that are already shaping what regulators expect inside dossiers.
If your submission pipeline still relies on copy-paste assembly, structured data requirements will expose that gap faster than any audit.
How teams design data ownership, metadata, and versioning
Structured data only works if your team defines who owns each data element and how changes get tracked. Without clear metadata governance and version control, structured submissions create new inconsistency risks. Build your data architecture so that each element has a single source of truth and a clear change history that auditors can follow.
What to prioritise first to avoid a big-bang migration
Start with high-frequency submission components like product information, labels, and clinical summaries. Migrating these to structured formats first gives you the biggest efficiency return without disrupting your entire document management infrastructure at once.
4. Expand real-world evidence in approvals and safety
Real-world evidence (RWE) has moved from a supplementary data source to a core input in regulatory decision-making. Regulators are no longer content to evaluate products solely on controlled trial results when large volumes of patient-level data from clinical practice are available and accessible.
Why regulators lean harder on post-market evidence
Controlled trials answer narrow questions under carefully managed conditions. Once a product reaches the market, regulators need evidence of how it performs across diverse populations, in real clinical settings, and over longer timeframes than most trials allow. Agencies including the FDA and EMA have both published frameworks that formalise RWE’s role in benefit-risk assessments and safety monitoring. This shift is reshaping what the future of regulatory affairs looks like for lifecycle management teams.
How RWE supports label expansions and risk management
Label expansions and new indication filings are increasingly supported by RWE packages, especially where running a new randomised trial would be impractical or unethical. Your RWE submission needs to show not just the data, but how the evidence was generated, curated, and analysed in a way that a regulator can audit.
Where teams often fail on data quality and bias
The most common failure point is inadequate source data validation. Teams pull data from electronic health records or registries without fully characterising missing data, coding inconsistencies, or selection bias in the patient population. Regulators flag these gaps quickly, and they erode the credibility of your entire evidence package.
Treat your real-world data sources with the same rigour you apply to clinical trial data, because regulators now do exactly that.
How to build an RWE operating model that regulators trust
Your RWE operating model needs defined data governance, pre-specified analysis plans, and clear documentation of all analytical decisions before you start extracting data. Build your approach around reproducibility so that any regulator reviewing your work can trace every conclusion back to a documented, defensible step.
5. Run more decentralised and hybrid clinical trials
Decentralised and hybrid trial models are moving from pilot programs into standard practice across major sponsors and contract research organisations. As the future of regulatory affairs shifts toward more flexible evidence generation, your team needs to understand what these models demand from a compliance and oversight standpoint before you commit to them.

What decentralised trials change for oversight and compliance
These models distribute trial activities across multiple sites, home settings, and digital platforms, which fragments oversight responsibilities in ways traditional monitoring frameworks were never designed to handle. Your compliance architecture needs to account for how investigator oversight works when patients complete visits remotely, and how you document that oversight in a format regulators will accept.
How to manage vendors, devices, and remote data flows
You will likely work with a larger vendor ecosystem than you are used to, covering wearables, ePRO platforms, telehealth providers, and local laboratories. Each vendor introduces data flow complexity, and your vendor qualification and oversight programme needs to be detailed enough to satisfy both GCP requirements and data privacy obligations across jurisdictions.
What good looks like for consent, privacy, and monitoring
Electronic informed consent processes need to meet the same standards as paper-based consent, with clear documentation of how subjects received, understood, and agreed to the information. Remote monitoring plans must specify how you detect data integrity issues and protocol deviations without routine on-site access.
Your consent and monitoring documentation needs to hold up under the same scrutiny as any in-person trial, not a lower standard.
How to keep protocols stable while adapting operations
Operational flexibility should not mean protocol instability. Define which operational elements sit outside the protocol so your team can adapt logistics without triggering formal amendments, and document those boundaries clearly in your trial master file from the outset.
6. Treat cybersecurity and data integrity as core compliance
Cybersecurity has crossed from the IT team’s responsibility into the core of your regulatory compliance programme. Regulators are now treating cyber vulnerabilities as direct risks to patient safety and data integrity, which means your compliance strategy needs to account for security controls, incident response, and supplier risk in the same breath as GCP and GMP obligations.
Why regulators now scrutinise cyber risk as patient risk
Agencies including the FDA have published guidance linking cybersecurity failures to product safety risks, particularly for connected medical devices and digital health tools. When a breach corrupts trial data or delays a safety signal, the patient impact is real. The future of regulatory affairs is one where your cyber posture is assessed during inspections alongside your quality systems, not separately.
Treat a cybersecurity gap the same way you would treat a data integrity gap: both carry enforcement risk.
How to protect trial data, safety systems, and submissions
Your access controls, encryption standards, and audit logging need to cover every system that touches regulated data, including third-party platforms used for remote trials or electronic submissions. Document your controls formally so that any inspector can follow the chain of protection from data entry to archive.
What to document for audits, incidents, and supplier risk
Keep a current record of every supplier with access to regulated data, their security qualifications, and the contractual obligations you have placed on them. Incident logs need to capture what happened, how you contained it, and what corrective action followed, in a format your quality management system already supports.
How to build security into validation and change control
Security requirements belong in your validation protocols and change control assessments from the start, not added after functional testing is complete. Each time a system or supplier changes, your risk assessment should explicitly address the security implications before you close the change record.
7. Accelerate reliance, work-sharing, and harmonisation
Reliance pathways and work-sharing arrangements are changing how regulatory teams plan global submissions. The future of regulatory affairs depends increasingly on your ability to leverage one agency’s assessment work to support approvals in other markets, reducing both time and cost across your portfolio.

How reliance pathways reshape global regulatory strategy
Regulatory agencies across the APAC region, including Australia’s TGA, actively participate in reliance and work-sharing frameworks that allow them to reference assessments from trusted reference agencies like the EMA or FDA. Your global strategy needs to account for these pathways from the start, not as an afterthought once your primary submissions are lodged.
Build reliance assumptions into your regulatory strategy document before you finalise your lead agency submission timeline.
What changes for planning, sequencing, and dossier design
Your submission sequencing decisions now carry more weight than they used to. If a reference agency’s assessment timeline slips, your reliance-dependent submissions slip with it. Dossier design also needs to anticipate jurisdiction-specific module requirements so you are not rebuilding core content from scratch for every market.
Where regional differences still force local work
Reliance does not eliminate local obligations. Markets including China, Brazil, and several Southeast Asian countries require country-specific data packages, local labelling formats, and in some cases local clinical data that no reference assessment can satisfy. Your team needs a clear map of where reliance applies and where it does not before you commit resource plans to leadership.
How teams avoid duplicated answers and conflicting commitments
When multiple agencies ask overlapping questions during parallel reviews, your responses need to stay consistent and cross-referenced across jurisdictions. Conflicting answers create credibility problems that are very difficult to walk back, so assign a single owner for each regulatory question across your global response coordination process.
8. Regulate advanced therapies with tighter lifecycle evidence
Cell, gene, and RNA therapies are pushing regulatory frameworks into territory they were not built to handle. The future of regulatory affairs in this space means working with living, complex products where the evidence requirements evolve alongside the science, often faster than guidance can keep up.
Why cell, gene, and RNA therapies stretch existing frameworks
These therapies do not behave like small molecules. Biological variability, manufacturing sensitivity, and long-term durability questions sit outside what traditional approval pathways were designed to address. Regulators including the EMA and FDA have published specific frameworks for advanced therapy medicinal products, but substantial gaps remain where your team must build the evidentiary logic from first principles.
Your regulatory strategy for an advanced therapy needs to treat evidence generation as a continuous lifecycle activity, not a pre-approval sprint.
How regulators assess comparability and manufacturing changes
Manufacturing changes in advanced therapies carry a higher regulatory burden than in conventional biologics because small process shifts can alter product quality in ways that are difficult to reverse or fully characterise. Your comparability packages need to include functional assays, potency data, and clinical bridging arguments that give reviewers confidence the product reaching patients matches what was studied in trials.
What teams must prove on long-term follow-up and safety
Regulators expect structured long-term follow-up programmes covering durability of effect, delayed adverse events, and persistence of modified cells or vectors in patients. Your safety monitoring plan needs to define collection intervals, endpoints, and escalation criteria that satisfy both the approval condition and your internal pharmacovigilance obligations.
How to plan for post-approval commitments from day one
Build your post-approval commitment register into your regulatory plan before your first submission, not after conditional approval is granted. Assign owners to each commitment, set realistic delivery timelines, and document your resourcing assumptions so that commitments you make to regulators are ones your team can actually deliver.
9. Bring manufacturing innovation into the regulatory file earlier
Manufacturing technology is outpacing the regulatory guidance designed to govern it, and that gap creates risk for teams that treat regulatory filing as a downstream activity. In the future of regulatory affairs, the expectation is that your regulatory strategy and manufacturing development programme run in parallel, not sequentially.
Why continuous manufacturing and automation move faster than guidance
Continuous manufacturing and automated process controls are becoming standard across biologics and small molecule facilities, but most regulatory frameworks were written with batch processing in mind. Your regulatory team needs to engage with manufacturing science early enough to shape the control strategy documentation before the process is locked, not after it is running at commercial scale.
How digital twins and process analytics change control strategies
Digital twins and real-time process analytical technology let manufacturers model and predict process performance in ways that traditional end-point testing cannot match. When you build these capabilities into your facility, your control strategy submission needs to reflect them accurately, including how models are validated, maintained, and used to support release decisions.
Document how your digital process models connect to your batch release criteria before your first regulatory submission references them.
What to show for validation, comparability, and release decisions
Regulators expect you to demonstrate that automated or continuous processes produce consistent quality outcomes with the same rigour applied to conventional manufacturing. Your validation packages need to cover process capability, edge-case performance data, and how your release testing aligns with real-time monitoring outputs.
How to align quality, regulatory, and engineering on one plan
Cross-functional alignment is where most teams lose time. Bring quality, regulatory, and engineering together around a single integrated development plan so that manufacturing changes trigger regulatory assessments automatically, not as a separate downstream task your team scrambles to complete after decisions are already made.
10. Build sustainability and supply chain resilience into compliance
Regulators and procurement teams are increasingly treating environmental impact and supply chain continuity as compliance issues, not just operational preferences. If your regulatory strategy still treats sustainability as a separate reporting exercise, you are already behind where the future of regulatory affairs is heading.

Why environmental impact and local resilience now shape regulation
Regulatory agencies and government procurement policies in Australia and across the EU are raising expectations for environmental accountability across the product lifecycle. Disruptions from recent global supply shocks have also pushed local sourcing and continuity planning firmly onto regulators’ radar, particularly for critical health and financial sector inputs.
Build your supply chain resilience argument into your compliance documentation, not your marketing materials.
What changes for materials, packaging, and waste controls
Your materials selection, packaging formats, and waste disposal records now carry regulatory weight in a way they did not five years ago. Regulators expect you to document not just what materials you use, but why, and how your choices align with applicable environmental standards and restrictions on hazardous substances.
How to evidence supplier oversight and continuity planning
Your supplier qualification programme needs to cover continuity risk alongside the standard quality and compliance criteria. Document alternative sourcing options, buffer stock policies, and escalation protocols so that any inspector can see you have assessed single-source dependencies and geographic concentration risks before they become a problem.
How to avoid green claims that trigger enforcement risk
Regulators and consumer protection agencies are scrutinising unsubstantiated environmental claims more aggressively than before. Any sustainability language in your labelling, submissions, or marketing needs to be backed by documented evidence that matches the specific claim, using defined metrics rather than broad or vague assertions.
11. Put patients at the centre of benefit-risk decisions
Patient engagement has moved from a consultation exercise to a core evidentiary requirement. Regulators are now asking development teams to show that patient perspectives shaped the evidence plan from the start, not that patients were consulted after the study design was finalised. In the future of regulatory affairs, teams that build patient input into their development logic early will have a structural advantage in benefit-risk discussions.
How patient input changes endpoints and labelling decisions
When you engage patients before you lock your endpoints, you surface outcome measures that actually matter to the people using your product. That shifts labelling conversations from clinical surrogate markers toward patient-relevant functional outcomes that regulators find more compelling when assessing benefit-risk balance. Document how patient input directly shaped your endpoint selection so reviewers can trace that logic through your submission.
What regulators expect for patient-focused evidence quality
Agencies including the FDA and EMA expect patient-focused evidence to meet the same methodological standards as any other evidence in your dossier. Qualitative research, patient preference studies, and concept elicitation work need clear methodology sections, defined populations, and transparent analysis, not anecdotal summaries attached as appendices.
Treat patient evidence with the same documentation discipline you apply to clinical trial data.
How to run inclusive development without slowing delivery
Build patient advisory involvement into your development calendar rather than scheduling it around submission deadlines. Use existing patient registries and advocacy networks to reach diverse populations early, which reduces the risk of late-stage feedback that forces protocol amendments.
How to document patient insights so they influence decisions
Your benefit-risk framework needs a dedicated section that maps patient-reported priorities to your evidence package. Each insight should carry a source reference and a clear statement of how it shaped a regulatory decision, giving reviewers a traceable, auditable record.
12. Align regulatory strategy with pricing and value evidence
Regulatory approval and market access used to be separate workstreams, but that separation is now a liability. In the future of regulatory affairs, teams that treat pricing and value evidence as a downstream concern consistently hit late-stage roadblocks that erode the commercial return on years of development investment.
Why value and access questions arrive earlier in development
Health technology assessment bodies and payers are engaging earlier in development dialogues, often before phase III trials are designed. If your team waits until post-approval to build a value dossier, you have almost certainly locked in evidence gaps that no supplementary study can fully close by the time reimbursement decisions are due.
How regulators and payers diverge on evidence needs
Regulators and payers ask fundamentally different questions from the same data package. Regulators focus on safety and efficacy relative to a controlled comparator, while payers want comparative effectiveness against the actual standard of care in their market, often with a local patient population. Your evidence plan needs to satisfy both sets of requirements without designing trials that are too broad to answer either question well.
Map your payer evidence requirements against your regulatory evidence plan before you finalise your phase III protocol.
What to do with patient-reported outcomes and RWE planning
Patient-reported outcomes and real-world evidence should be pre-specified in your development plan with clear links to both your submission dossier and your value story. Build your RWE collection infrastructure early so that post-launch data accumulates in a format both regulators and payers will accept as fit for purpose.
How to prevent late-stage surprises that block reimbursement
Assign a cross-functional owner who sits across regulatory, market access, and medical affairs from phase II onward. Regular evidence gap reviews against payer criteria catch misalignments while you still have time to course-correct without amending a locked protocol.
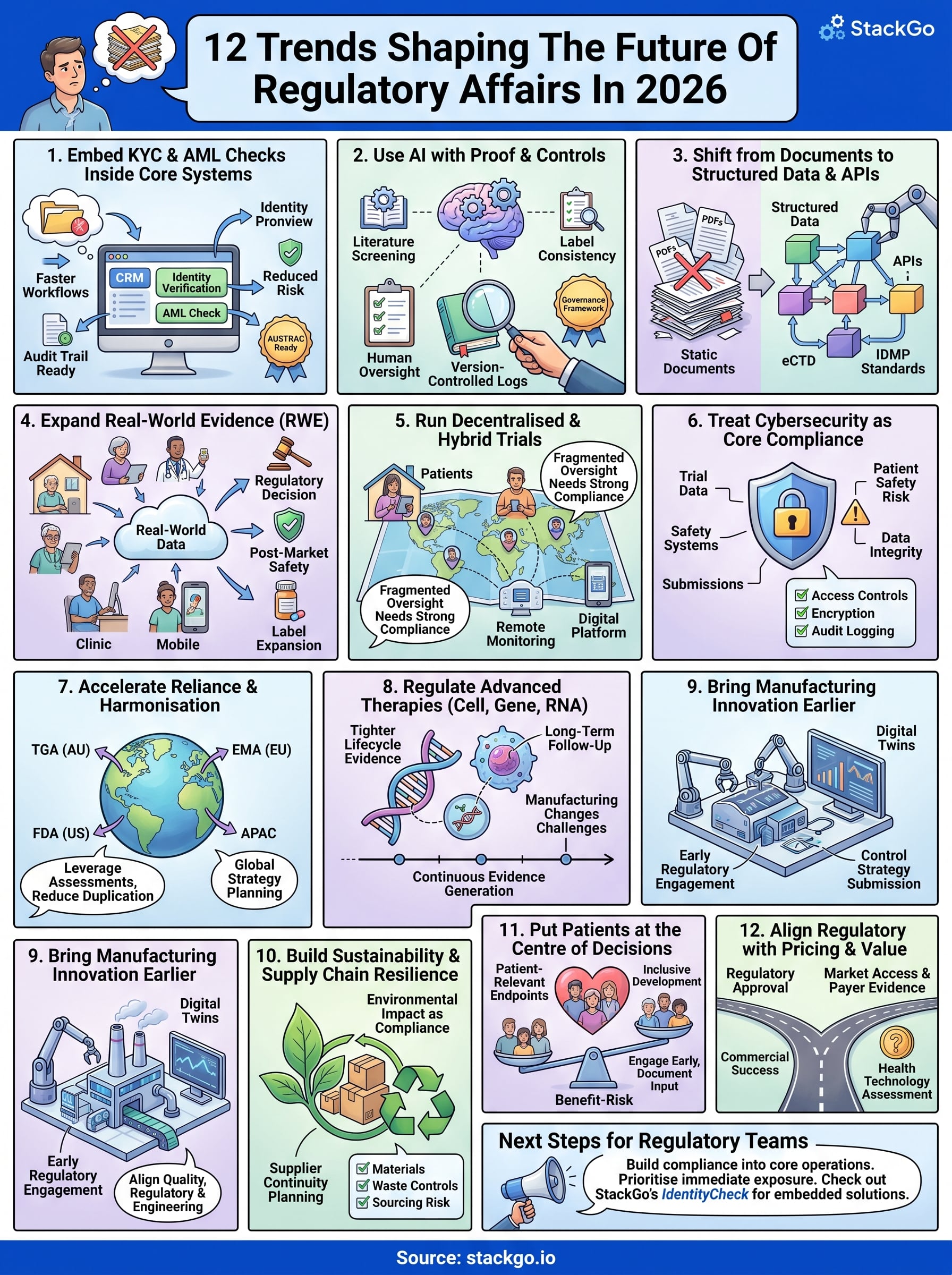
Next steps for regulatory teams
The trends across this list share one common thread: the future of regulatory affairs rewards teams that build compliance into their core operations rather than layering it on top. Whether you are managing KYC and AML obligations as an Australian accounting firm, running structured data migrations, or aligning regulatory strategy with payer evidence, teams that move first build durable advantages that slower-moving competitors struggle to close.
Start by identifying which of the 12 trends above creates the most immediate exposure for your business. Prioritise the areas where a gap directly threatens your ability to operate, onboard clients, or satisfy a regulator, then work outward from there. Your compliance stack needs to support that prioritisation, not slow it down. If embedded identity verification is your most pressing need, run a free test of IdentityCheck to see how it fits your existing systems before committing to a full rollout.









